 However, no further improvement was noted by 12 months postpartum. Then, by 6 months postpartum, the hiatus had improved and narrowed to return to an area comparable to that at 21 weeks’ gestation. In this study, the levator hiatus area was significantly larger at 37 weeks’ gestation and at 6 weeks postpartum compared with earlier pregnancy. This hiatus is the U-shaped opening in the pelvic floor muscles through which the urethra, vagina, and rectum pass ( Chap. In 300 nulliparas, they measured bladder neck mobility and the area within the urogenital hiatus during Valsalva. To assess this in part, Staer-Jensen and colleagues (2015) obtained transperineal sonographic measurements of the pelvic floor muscles at 21 weeks’ and 37 weeks’ gestation, and again at 6 weeks, 6 months, and 12 months postpartum. According to Nygaard (2015), vaginal delivery is a traumatic event. ( g) Birth of the anterior shoulder ( arrow).Many adaptive changes are required for pregnancy and for labor and delivery. ( f) Fetal head expression from birth canal. ( e) Movement of return (or external rotation of the fetal head) in which the frontal–occipital diameter is oriented along the oblique diameter left ( right), as similar to the one position that the head assumes the entrance pelvic. ( d) Translabial ultrasound image showing the complete rotation (internal rotation) and the full extent of the fetal head. ( c) An ultrasound image of translabial that displays the rotation of the head that has reached the ischial spines, and the diameter of the occipito-front is aligned with the anteroposterior diameter of the pelvis. ( b) Transabdominal ultrasound image showing the progression of the head toward the close medium and rotation ( right). ( a) Illustration of a transabdominal ultrasound showing the mechanism of commitment, the bending of the head down the narrow upper left oblique diameter according to the transverse ( right). This study provides evidence that digital assessment of fetal head station is unreliable. Undiagnosed “high” stations accounted for 22% of the errors made by residents, and 16% of those made by attending physicians. The mean error rate in the diagnosis of engagement was 12%, and this misdiagnosis was distributed equally between false-positives and false-negatives. Numerical errors occurred in 50–88% of cases for residents (average experience 2 years) and in 36–80% of cases for attending physicians (average experience 9 years). The error in the diagnosis of station was assessed by calculating the difference between the true station (established by sensors in the birth simulator) and that determined by the clinician’s fingers. A fetal head mannequin was placed in 11 different stations in a random order. He used a birth simulator with objectively defined stations and studied the reliability of clinical assessment of engagement and fetal station in 57 physicians (32 residents and 25 attending physicians). made an important contribution to this debate when he rigorously assessed the accuracy of station diagnosis with digital examinations. Recent studies, however, dispute these findings and found clinical examination of fetal descent and position to be subjective with high interobserver variation. In one study from the 1980s, repeatability of digital examinations was found to be acceptable. 
Traditionally, labor progression has been assessed by digital examination of cervical dilatation and fetal descent. Prolonged labor is defined when cervical dilatation crosses the “action line.” Some hospitals use partographs from the Dublin school of “active management of labor” and expect one-cm dilatation/hour (the slope of the alert line), whereas other hospitals define prolonged labor when cervical dilatation is <1.2 cm/h in nulliparous women and <1.5 cm/h in parous women. Philpott suggested in 1972 to use “alert lines” and “action lines” (4 h from the “alert line”) in partographs to evaluate labor progress, and WHO has adopted this method. He has documented a strong correlation between cervical dilatation and station and an association between high station at arrest of labor and adverse outcome. In 1954, Friedman introduced the partograph. 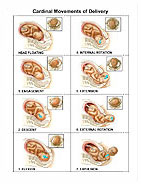
Minus five corresponds to the pelvic inlet, zero to the level of the ischial spine, and plus four corresponds to the pelvic floor (Fig. 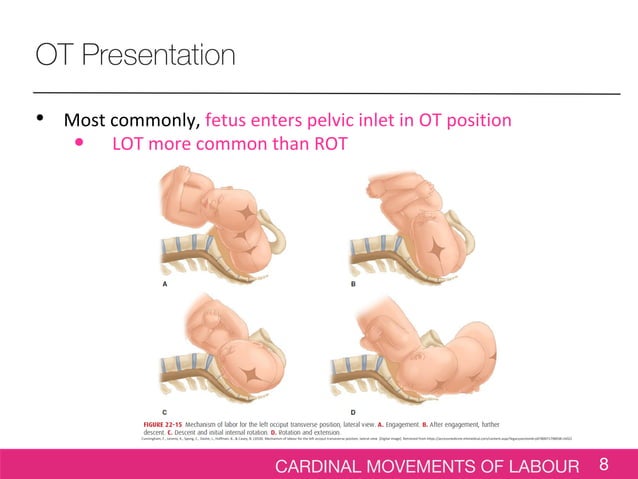
The fetal descent in the birth canal is assessed by vaginal digital examinations and related to the ischial spine (Fig. Müller first described the concept of station in 1868. The fetal lie can be longitudinal or transverse, presentation describes the lowest fetal part in the birth canal, position means how the fetus is rotated, and station refers to the level of the presenting part in the birth canal. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
